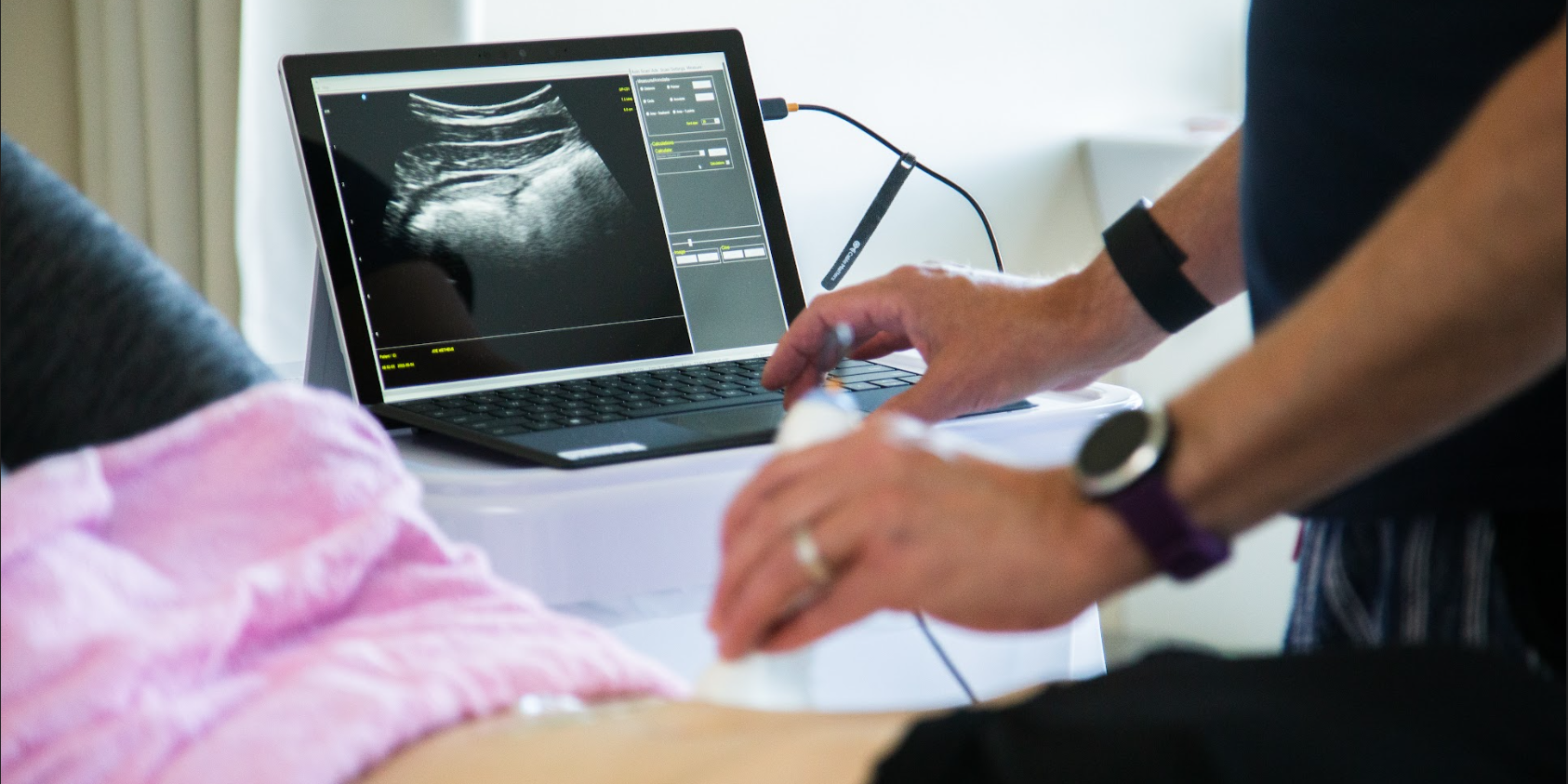
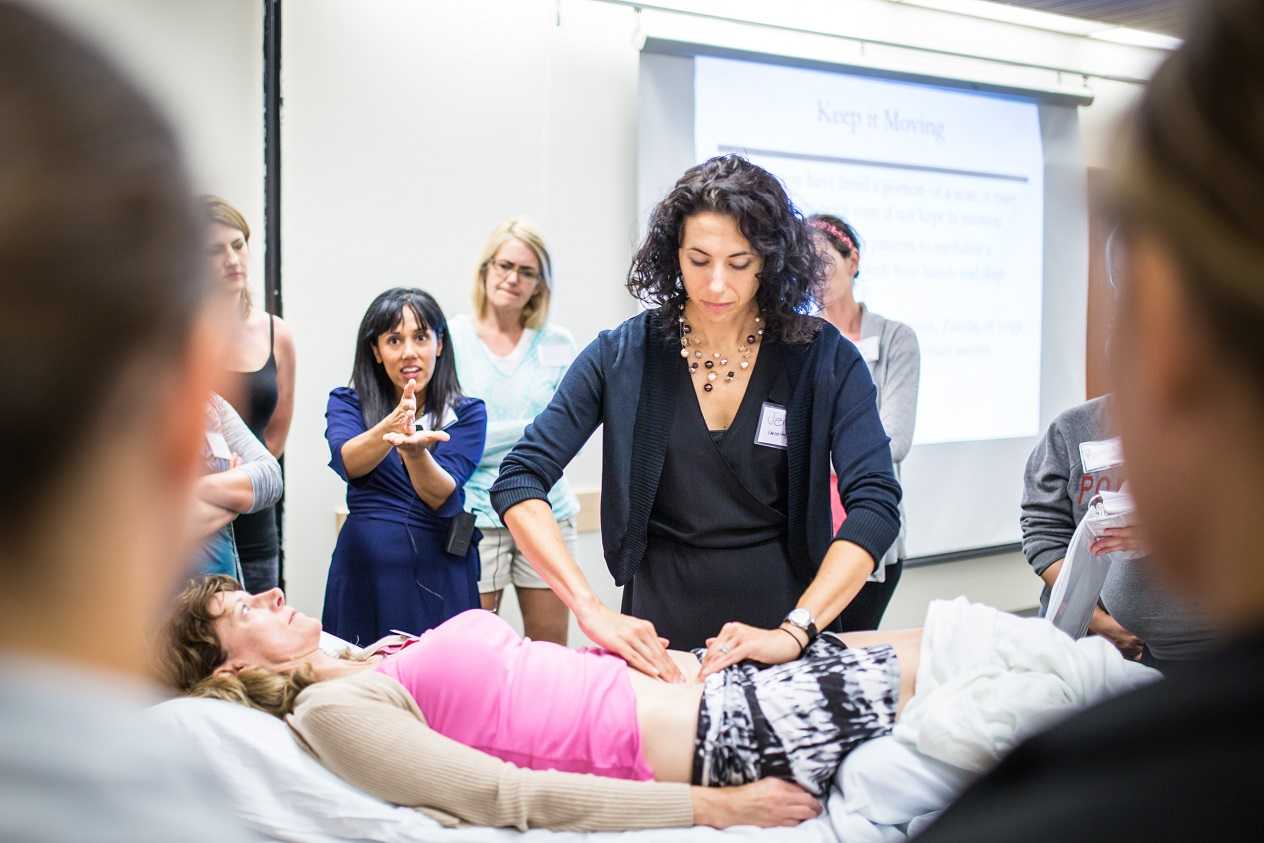
In his famous book Light on Yoga, B K S Iyengar describes pranayama as “extension of breath and its control”1. Pranayama includes all aspects of breathwork: inhalation, exhalation, and breath retention. As clinicians treating pelvic floor dysfunction, we emphasize the importance of breathing as a critical component of rehabilitation. Physical therapists Paul Hodges (et al) and Julie Wiebe describe a piston-like relationship between the diaphragm and pelvic floor2,3. Pranayama, or conscious breathing, can enhance this relationship, especially if there are holding patterns in the pelvis. On inhalation, the pelvic floor muscles and diaphragm move caudally. On exhalation, the pelvic floor muscles and diaphragm move cranially4. As physical therapists, we instruct patients to use the breath in coordination with the pelvic floor muscles to obtain optimal stability and continence.

Pelvic organ prolapse and urinary/fecal incontinence are often caused by a lack of tonic support and muscular strength of the pelvic floor, core and surrounding pelvic girdle musculature5. Optimal pelvic floor support from adequate strength, core stability, and neuromuscular control allows for continence and organ support. For optimal core stability, there must be coordination and strength of all components of the deep core musculature – pelvic floor muscles, transverse abdominals, multifidi, and diaphragm6. The “Soda Pop Can Model of Postural Control”, conceptualized by Mary Massery, illustrates how the pressure system of an aluminum soda can maintains the stability of the structure7. Loss of support can happen at the top (i.e. tracheotomy), front (i.e. diastasis recti abdominus), back (i.e. disc herniation), or bottom (i.e. pelvic organ prolapse or incontinence). A “leak” in the structural integrity could affect postural control, core stability, and continence. This concept underlines the importance of breath retraining as one aspect of our treatment plan.
Pranayama gives your patient a strategy to decrease sympathetic nervous system overactivity and encourages the parasympathetic response. According to Diane Lee, common areas of rigidity of movement/holding patterns include lateral and posterior-lateral expansion of the ribcage during inhalation8. Mindful pranayama encourages the student to explore diaphragmatic breathing without gripping in the chest and ribcage.
Examples of pranayama
Dirgha
Dirgha is the Three-Part Breath. Inhale, allowing the belly to fill. If your patient finds this challenging, try a book on the belly when supine or try breathing in quadruped. The second part of dirgha is expanding the ribcage, followed by the collarbones to floating up. After trying this for 10 breath cycles, stop and recognize any new sensations or softening in the body. I recommend my patients set an alarm to go off every hour to remind them to move and breathe.
Ujjayi
Ujjayi is known as the Ocean breath. It sounds like you have one ear to a giant seashell. Raise one hand in front of the mouth and pretend to fog a mirror with an inhalation and exhalation. Recreate the same action at the back of the throat, but now with the mouth closed. This breath should sound similar to the signature sound of the Star Wars villain Darth Vader. Perform this breath with any warm-up or asana while layer this breath onto Dirgha.
Letting Go Breath
Letting Go Breath can be a great reset. Inhale through the nose. Gentle exhale with an audible sigh through the mouth. It’s a quick check in to access instant awareness to the areas in the body that habitually hold tension.
Integrating into the clinic
Depending on the patient, I may not reference the Sanskrit name of the pranayama in the clinic. If the client is seeking a private yoga session, the names of these pranayamas will come up. As always, I meet my patient where they are and don’t push or recommend yoga practices that they are not interested in.
Breathwork can be performed supine while hooked up to biofeedback, sitting with their hands on their abdomen and chest, or standing moving their arms through abduction during inhalation. These examples are only the beginning of possibilities!
1) Iyengar BKS. Light on Yoga: Yoga Dipika. Schocken; 1995.
2) Sapsford RR, Richardson CA, Maher CF, Hodges PW. Pelvic floor muscle activity in different sitting postures in continent and incontinent women. Arch Phys Med Rehabil. 2008;89(9):1741-1747.15.
3) Julie Wiebe, Physical Therapist | Educator, Advocate, Clinician. 2015; http://www.juliewiebept.com/.
4) Talasz H, Kremser C, Kofler M, Kalchschmid E, Lechleitner M, Rudisch A. Phase-locked parallel movement of diaphragm and pelvic floor during breathing and coughing-a dynamic MRI investigation in healthy females. Int Urogynecol J. 2011;22(1):61-68.
5) Sapsford R. Rehabilitation of pelvic floor muscles utilizing trunk stabilization. Man Ther. 2004;9(1):3-12.
6) Lee DG. The Pelvic Girdle: An integration of clinical expertise and research, 4e. Churchill Livingstone; 2010.
7) Massery M. THE LINDA CRANE MEMORIAL LECTURE: The Patient Puzzle: Piecing it Together. Cardiopulm Phys Ther J. 2009;20(2):19-27.
8) Lee DG. The Pelvic Girdle: An integration of clinical expertise and research, 4e. Churchill Livingstone; 2010.