Male chronic pelvic pain (CPP) is well-known to be associated with sexual health impairments including, but not limited to, pain limiting sexual activity, premature ejaculation, erectile dysfunction. In addition to potential interference in sexual activity due to pelvic pain associated alteration in libido and function, does CPP affect sperm health? According to a systematic review and meta-analysis published this year, semen parameters are impacted in men who present with chronic pelvic pain. 12 studies were utilized, including nearly 999 cases and 455 controls. Semen parameters studied included seminal plasma volume, sperm concentration, total sperm count, motility, vitality, and morphology. Men diagnosed in the studies with CPP or chronic pelvic pain syndrome (CPPS) met the NIH criteria for the condition.
The results of the analysis indicate that sperm concentration, percentage of progressively motile sperm, and morphologically normal sperm in patients with CPP/CPPS were significantly reduced when compared with controls. Semen volume was higher in the CPP pain group than in controls, and the results suggested no significant difference in sperm total motility, sperm vitality, and total sperm count. How do these factors affect fertility? The authors point out that semen parameters are "the mainstay of male fertility and reproductive health assessment" and and that the percentage of morphologically normal sperm is an indicator of male fertility potential. While the sperm concentration was identified to be lower in male patients who have CPP, the semen volume being elevated may affect these numbers. Sperm motility, being necessary for fertilization, would logically be a factor in potential impairment of fertility.
The authors discuss the possibility that an inflammatory response associated with chronic pelvic pain, or an autoimmune response against prostate specific antigens factor into the alterations in semen analysis observed in men who have chronic pelvic pain. While the issue of fertility and pelvic pain is controversial, and not entirely understand, we can hypothesize about local factors affecting pelvic and sexual health, as well as autonomic nervous system implications mediated by the chronic pain state. As science aids in the understanding of the mechanisms affecting semen parameters, pelvic rehabilitation professionals will continue to address the potential causes of the dysfunction: nervous system dysfunction such as anxiety, depression, hormonal regulation, and neuromuscular pain states that may affect local blood and lymph flow (and therefore affect cellular nutrition and removal of waste products of cellular metabolism). If you are interested in learning more about male anatomy, sexual dysfunction, pelvic pain, and incontinence, come to the Male Pelvic Floor Function, Dysfunction, & Treatment continuing education course in Tampa in October!
This post was written by H&W instructor Allison Ariail PT, DPT, CLT-LANA, BCB-PMD. Allison will be instructing the Pelvic Floor Level 1 course Boston this October.

Several weeks ago some of my fellow faculty members and I were discussing the resting tone of the pelvic floor. These days we take it for granted that we know there is constant low-level activity in the pelvic floor and anal sphincter in order to provide continence. However, how did this information come about? I took it upon myself to do some research to find out the beginnings of this knowledge. What I found was interesting and thought I would share.
In the late 1940’s and early 1950’s the belief was held that the pelvic floor and external anal sphincters were inactive at rest, like other striated muscle throughout the body. Activity was believed to be initiated by afferent impulses from the rectal ampulla and anal canal. In 1953 Floyd and Walls found activity in the external anal sphincters at rest, even during sleep. In 1962 Parks, Porter, and Melzak published a study examining the pelvic floor muscles and the external anal sphincters using electromyography recordings. They also found activity in these muscles at rest. They hypothesized the activity was maintained by spinal reflex. These researchers looked at the activity in a healthy population, a paraplegic population, and a population that had undergone a rectal excision. When examining the paraplegic population (all subjects had complete SCI injuries above L3), they did identify activity of the pelvic floor at rest.
With respects to the rectal excision population, they examined patients whose rectums were removed, but the somatic muscles, external sphincters, and the levator ani remained with innervation intact and the muscles were sutured to provide a muscular pelvic floor. These patients also exhibited activity in the pelvic floor and anal sphincter at rest. These patients were important to the study in order to rule out that the reflex was not coming from somewhere in the rectal wall. Additionally, these researchers discovered this resting activity that was present the anal sphincter was inhibited during defecation in response to a certain degree of rectal distension.
So what did all of this new information mean to these researchers? It meant that the pelvic floor and external anal sphincter were unique due to the fact they were activated at rest, and without this activation continence would not be maintained. They determined the activation to be reflex and termed it “postural reflex of the pelvic floor.” Additionally, they termed the inhibition due to rectal distension “the rectal inhibitory reflex,” which also was due to a reflex arc. This new information was groundbreaking for the time and lead to other research that provided us with the knowledge that we have today! Thank goodness for these researchers as well as the many others who have furthered the advancement of knowledge about the pelvic floor!
Learn more about Allison and the Pelvic Floor Series by visiting our website!
1. Floyd, Walls. Electromyography of sphincter ani externus in man. J. Physiol. 122: 599, 1953.
2.Parks, Porter, Melzak. Experimental study of the reflex mechanism controlling the muscles of the pelvic floor. Dis. Colon Rectum. 5 (6): 407. 1962.
This post was written by H&W instructor Carolyn McManus, PT, MS, MA. Carolyn will be instructing the course that she wrote on "Mindfulness-Based Biopsychosocial Approach to the Treatment of Chronic Pain" in Seattle this November.

I have taught Mindfulness Based Stress Reduction at Swedish Medical Center (SMC) since 1998. Over the years I have had many healthcare providers take the course and have long thought it would be wonderful to tailor a program specifically for healthcare professionals. I had the opportunity to do so this summer when, along with my colleague Diane Hetrick, PT, we designed and taught Mindfulness and Compassion Cultivation Training for physicians at SMC. The course was a great success. Physicians reported one of the most popular components of the program were our “on the spot” mindful practices. These are simple, easy-to-do strategies that any provider can employ to center, calm the body and steady the mind during a busy workday. They not only help reduce stress, but can influence brain activation to promote better decision making.
Research shows, under stress conditions, the amygdala activates stress pathways in hypothalamus and brainstem, evoking high levels of noradrenaline and dopamine release, impairing prefrontal cortex function. (1) Research also shows mindful practices reduce stress-related brain activity and improve executive functioning. (2, 3) I am delighted to share these powerful and practical “on the spot” mindful practices in my November course. My intention is for participants to have mindfulness skills to use for their own well-being the minute they walk in their clinic door on Monday.
Learn more about Carolyn's course Mindfulness-Based Biopsychosocial Approach to Chronic Pain and join her in Seattle this fall!
1. Arnsten AF. Stress signaling pathways that impair prefrontal cortex structure and function. Nat Rev Neurosci 2009:10(6):410-422.
2. Holzel BK, Carmody J, Evans KC, et al. Stress reduction correlates with structural changes in the amygdala. Soc Cogn Affect Neurosci. 2010;5(1):11–17.
3. van den Hurk PA, Giommi F, Gielen SC, et al. Greater efficiency in attentional processing related to mindfulness meditation. Q J Exp Psychol (Hove) 2010;63(6);1168–1180.
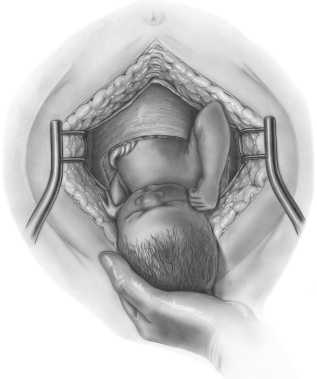
When a woman is interested in a trial of labor after previous cesarean delivery (TOLAC), she and her health care providers will consider the pros and cons of delivery methods. Researchers have aimed to predict success with vaginal birth after cesarean section (CS), with the intention of limiting the risk factors for both the mother and the fetus. A failed trial of labor following a CS may be associated with higher maternal and perinatal morbidity, according to the American College of Obstetricians and Gynecologists (ACOG) practice bulletin.
The goal of a study published last year was to develop a model for predicting success in women desiring a vaginal birth after cesarean (VBAC) section. All women had one prior CS, all were carrying singletons. Transvaginal ultrasound was utilized to evaluate the Cesarean scar (CS) at 11-13, 19-21, and 34-36 weeks' gestation in 320 women. The measurement of the scar was termed residual myometrial thickness (RMT), and the measurements also included the change in RMT from the 1st to 2nd trimester. With increased evidence that CS healing and myometrial thickness in the lower uterus may improve success with VBAC, this study is the first to assess scar dimensions across the first and second trimesters.
The CS scar was visible in 89% of the women. Of these, 153 of the 284 were excluded from the prediction model development due to having had more than one prior cesarean delivery, so the hospital protocol of scheduling cesarean was followed. The remaining women were offered a vaginal birth trial, with 10 of the 131 undergoing CS prior to labor for varied reasons. The final count of women included in the analysis was 121, and of these cases, 74 had successful VBAC, 47 experience failed trials of labor, primarily due to fetal distress, failure to progress, or possible scar rupture. (In the women who did not have a visible scar, 82% had a successful vaginal delivery.)
The median residual myometrial thickness, or RMT, was higher in patients who had a successful VBAC. Clinical usefulness, according to the study, is that use of the model may lead to fewer emergency CS deliveries through identification of women who will be successful with VBAC.
The authors concluded that measurements of a CS, when applied to a mathematical model, can predict success of a vaginal birth after CS. This information may be very interesting to discuss with our referring providers, our colleagues, as well as our patients. Any research that sheds light on variables to predict success with a VBAC may promote vaginal deliveries and hopefully prevent emergency cesarean deliveries. Educating our patients so they can be more informed and advocate for themselves is a key role. While we are always mindful of not overstepping our scope of practice, such as advising a woman if she should choose one method of delivery over another, the information about the scar thickness in predicting VBAC success may be very useful to both her and providers. For more information about peripartum issues, check out our Peripartum Course Series on the course page. There is still time to sign up for the Care of the Postpartum Patient continuing education course later this month in Chicago!
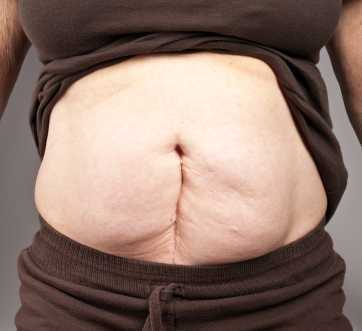
A systematic review aimed to identify the burden of the most significant complications of postoperative abdominopelvic adhesions. Of the nearly 200 studies included in the review, the following categories were included: small bowel obstruction (n=125), difficulties during subsequent operation (n=62), infertility (n=11), and chronic pain (n=5). The incidence of postoperative small bowel obstruction, assessed among nearly 108,000 patients in 92 studies, was 9% overall. The incidence of adhesive small bowel obstruction was 2.4% and was highest in pediatric and in lower gastrointestinal tract surgery. The authors report a high rate of chronic abdominal pain in patients who were followed after lower gastrointestinal tract surgery, with adhesions identified as a significant cause of this pain. Following colorectal surgery for small bowel disease, pregnancy rates were found to be dramatically lower than the pregnancy rates in those who were medically treated. Additionally, patients who have had a prior surgery may require additional time in a subsequent procedure due to scar tissue, and adhesiolysis, used to break up adhesions, can lead to bowel injury.
Patients with postoperative adhesions, according to the systematic review, are most often treated by providers other than the one who did the surgery; the lack of awareness of the complication may be one reason that the incidence of adhesions is underestimated. The value of being aware of the higher incidence of postoperative adhesions may be in early recognition of a complication, surgical decision-making, and patient counseling. While the research is young in relation to adhesions and pelvic rehabilitation, one study that we previously discussed in the blog addresses visceral mobilization techniques in an animal model. While the animal model research is promising, there are numerous case reports describing the positive effects of visceral mobilization techniques for abdominopelvic pain, and therapists always report on the equally positive changes to their clinical practice outcomes after adding visceral techniques to their toolbox.
There are 2 upcoming opportunities to learn visceral mobilization: Level 1 in Scottsdale covering the Urologic system and Level 2 in Boston covering the reproductive system.
One of the questions we frequently receive at the Institute is "Do you have any research about ___________?" At times, therapists are looking for information that can help with patient care, or they might be looking for support in a claims denial letter, or foundational material for a presentation. If you have been taught how to find articles, this may seem like a simple task. Many of us therapists went to school when the only use of a computer was for word processing, if we were lucky enough to have progressed from the typewriter or even the electronic typewriter. (Imagine no Google, no Wikipedia, and no Amazon to purchase textbooks!) There are basic search skills that can be shared so that every person interested in a particular topic can find recent articles in free search engines. While the full article may not be available, many times you will have access to full articles that synthesize recent works. (One website that you can use that offers full text article access is PubMed Central.) If you are not interested in reading articles, but prefer to read a scholarly summary of a health topic, check out www.uptodate.com, where you can subscribe to have full access to excellent evidence-based summaries. You can read through the reference lists on the site as well to see if there is a resource that you want to track down.
One method of finding articles is to go to www.googlescholar.com. In the search bar, type in the topic you are interested in, such as "urinary incontinence." You will then be provided with a list of all articles that have urinary and/or incontinence in the title or in the key words of the research. An even more refined way to conduct your search is by using Boolean terms, in which you connect your search words by "AND" or other key terms. To see this in action, let's say you want to know if there is any research about urinary incontinence and prostatectomy surgery. Try completing a google scholar search by typing in the following: "urinary incontinence" AND "prostatectomy". (Be sure to use the quotation marks and type the word "AND" in capital letters.) You will see that you come up with some very nice articles about the specific topic you searched. To make sure you are looking at recent articles, go to the left side of the search page and under the words "Any time" choose an option such as "Since 2010" so that you are seeing articles from within the last 5 years. Next, maybe you want to know if there is evidence for rehabilitation. Add the word rehabilitation, like this: "urinary incontinence" AND "prostatectomy" AND "rehabilitation". You will see that you now have even more results specific to rehabilitation of the condition. On the right side of the page you might see a link that starts with [PDF] where, if you click on it, you will usually be brought to the full article rather than just the abstract. If you see an article that you think fits your search, you can also click on "Related articles" located under the brief description of the article.
Being able to look up articles serves many purposes, including staying updated on patient care, and discussing evidence with peers, providers, and patients. Another valuable reason to find your own research is when studying for certification exams such as the Pelvic Rehabilitation Practitioner Certification (PRPC). On the PRPC certification page on our website, you can find a list of some articles for which we have added links. (Remember that there is no need to print out articles anymore! Save a tree and simply save the articles as a PDF file. You can name the article by the author's last name, year and main topic, and store in a folder on your computer so it is easy to access- no file drawer required!) If you are thinking about taking the PRPC exam, there is no time like the present to get your application put together! The deadline for applying is October 1 of this year, with the test taking place in the first couple weeks of November. Personally, I have enjoyed reading the blog posts introducing therapists who have earned their PRPC title- the reasons for seeking the distinction are very interesting and meaningful. We would love to see your name on the list of certified therapists, so check out the details on the website and contact us if you have any questions about the PRPC application process!
In an article describing vascular dysfunction in women with chronic pelvic pain (CPP), Foong and colleagues describe the common finding of pelvic venous congestion. This study aimed to determine changes in microcirculatory function in women with chronic pelvic pain compared to controls. Eighteen women presenting with chronic pelvic pain of at least 1 year and 13 women without pelvic pain or congestion were evaluated for isovolumetric venous pressure, miscrovascular filtration capacity, and limb blood flow. All women were of reproductive age, menstruating regularly, and measurements were made during the mid follicular and the midluteal stages of the same 28 day cycle. The 18 women with CPP fit previously established criteria for pelvic congestion.
The women in the patient group were re-evaluated at 5-6 months following treatment for pelvic congestion, with treatment including medication-induced suppression of ovarian function for 6 months, and in 4 patients, hysterectomy and bilateral salpingo-oopherectomy. All of the patients received daily hormone replacement therapy (Premarin and Provera) "…to minimize the hypo-oestrogenic effects of treatment."
Findings of the research include an elevation in isovolumetric venous pressure, or Pvi in women with CPP compared to controls. Interestingly, there were no changes related to menstrual cycle in measures of microvascular filtration capacity and and limb blood flow. The conclusion of this study is that women with chronic pelvic pain may present with systemic microvascular dysfunction. The noted increase in Pvi "…may be attributable to systemic increases in post capillary resistance secondary to neutrophil activation." Following treatment for pelvic congestion, the value changes in isovolumetric venous pressure were no longer present.
This research highlights the noted changes in microcirculatory function in women with chronic pelvic pain. The obligatory chicken and egg conversation weighs in: does pelvic congestion lead to pelvic pain, or does pelvic pain always precede pelvic congestion? While the answer is probably that either condition can cause and perpetuate the other, as pelvic rehabilitation providers, our first thought might be: what would the research outcomes be if the treatment were not medication-induced ovarian suppression or surgery, but therapy directed to the pelvic pain and congestion? The Institute offered, for the first time last year, a course that allows the therapist to address pelvic pain through treatment of pelvic lymphatic drainage. The Lymphatic Drainage for Pelvic Pain continuing education course is a 2-day class instructed by Debora Hickman, a certified lymphedema therapist. Sign up now to save your seat in October in San Diego, and if you can't make this course, contact us to let us know you are interested in this special topics course, and we will keep you informed of any new course bookings!
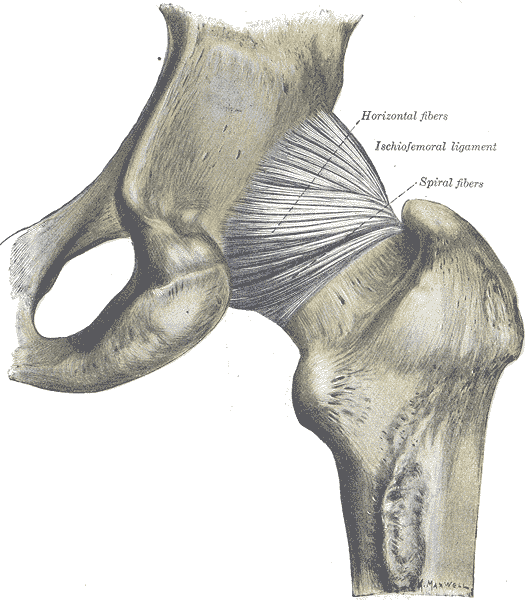
What structures may be implicated in posterior hip pain in the athlete? This question is addressed in a comprehensive article that can be accessed here. Complaints of posterior hip pain are increasingly common, and the differential diagnosis can include a variety of conditions and structures. The differential diagnosis of posterior hip pain may include hip extensor or hip rotator muscle strain, femoroacetabular impingement, proximal hamstring rupture, piriformis syndrome, and referral from the lumbar spine or sacroiliac joint, and systemic conditions such as cancer or infection, according to the article. To this list, could we add sciatic and other nerves in the buttock and pelvic floor, ischial injuries or ischial bursa irritation? With lists that include both systemic dysfunction and a variety of potential neuromusculoskeletal causes of posterior hip pain, the therapist must have a comprehensive ability to apply clinical reasoning, expert interview, and solid clinical examination and evaluation skills.
Posterior hip pain is only one type of hip pain, and one complaint within the world of pelvic pain. How does the therapist keep sharp tools for diagnosing musculoskeletal conditions, other connective tissue dysfunctions, as well as screen for disease conditions and other dysfunctions that can mimic hip or pelvic pain? Herman & Wallace has increased our offerings of courses towards differential diagnosis of hip and pelvic pain, including Biomechanical Assessment of the Hip & Pelvis, taught recently by Steve Dischiavi. (Stay tuned for Steve's upcoming course schedule!)
Another continuing education course that offers excellent opportunity to fine tune your skills in Differential Diagnosis of Pelvic Pain is coming up in October in Connecticut. The course is instructed by Peter Philip, who completed his Doctor of Science degree on the topic of Differential Diagnostics of Pelvic Pain. In addition to learning detailed anatomy and palpation skills, the participant can take away from the course a better understanding of embryology, the somatic and autonomic nervous system, and pelvic conditions that may be caused by or influenced by pelvic pain. The course will include both internal and external pelvic muscle examination techniques. With seven labs scheduled in this continuing education course, the participant will have abundant opportunities to practice instructed skills.
This post was written by H&W instructor Ginger Garner, MPT, ATC, PYT. Ginger will be instructing the course that she wrote on "Yoga as Medicine for Pregnancy" in New York this November.

The power of language is inarguable. The spoken word affects how we see, perceive, and interpret the world around us. Language can also influence our actions and behavior, especially toward people around us.
The power of language in health care is not only important, but critical in prenatal health. The language a provider uses can help or harm a mother’s confidence and even her beliefs about birth.
Action to recognize and respond to the importance of language in general health care began with People First Language (PFL) movement. PFL advocates for mindful use of language that identifies the person first, rather than identifying the person based on their disability. Advocacy groups first started the movement for children’s sake. Mother’s who had given birth to children with Down’s syndrome wanted their children to be recognized as people first, rather than by their disability.
An example of People First Language would be, “Beth is a child who has Down’s syndrome,” instead of “Beth is a Down’s (syndrome) child.”
The second statement can be dehumanizing, whether intentional or subconscious. The effects of being identified as a disability, rather than as a human being, are far reaching on psycho-emotional and physical health, and can project a negative connotation on the individual. Read more on People First Language
However, have you noticed that no such language is used for prenatal care?
The shameful statistics on American childbirth and mortality rates for mothers and babies is no secret, internationally. However, many US mothers may not realize that their likelihood of receiving poor prenatal care is so high. In fact, it is dangerously high. Read my post: American Childbirth: A Human Rights Failure?
However everyone, including health care providers who provide prenatal care, can have a powerful impact on improving childbirth in America.
How? Through language.
Yoga as Medicine for Childbirth & Postpartum courses I teach for Herman & Wallace Pelvic Rehabilitation Institute, language is a powerful part of the empowerment process for women. It is an integral part of the biopsychosocial model available to 21st century healthcare providers who use yoga in prenatal and postpartum care. Yoga can improve postpartum physical therapy care and help moms who want to have a natural childbirth. Yoga is also a powerful prenatal mind-body fitness aid as well and works to decrease pain across the journey of pregnancy and into postpartum. Read this post on Why Every Expectant Mom Needs Yoga.
Yoga is a mind-body practice that places paramount importance on language. In fact, yoga uses an entirely different language than biomedical prenatal or postpartum care. Yoga focuses on empowerment through language and action.
Prenatal care using women-centered language looks very different than the historically patriarchal driven vernacular that is still being used today. These statements describe the same situation, but have profoundly different effects on a woman and her confidence and ability to give birth. Consider these common scenarios from a perspective on The Power of Birth Language.
Which scenario would you rather give birth in:
“My doctor/midwife is going to let me use a birthing tub.”
VERSUS “My doctor/midwife supports my plan to give birth in water.”
“My doctor/midwife delivered my baby.”
VERSUS “I gave birth to my baby (in the are of ______).
The first scenario in each example takes power from the mother and negates her participation and involvement in pregnancy and birth. The first scenarios also place her in a dominator relationship under the authority and order of the health care provider.
The second scenario in each example recognizes that mothers should be full partners in their own healthcare, not subordinates without a voice. The second scenario also recognizes that birth should be women-centered, not healthcare provider-centric.
Woman-centered language can usher in a powerful shift in prenatal care, helping tip the scales toward the positive for birth reform in America. Adopting the mindfulness of an ancient system, like yoga, can likewise enrich and expedite the process of reclaiming the full power of birth.
To learn more about Ginger's Women-centered continuing education for health care providers seeking integrated care when working with women during pregnancy or postpartum, visit Yoga as Medicine for Childbirth & Postpartum and join her for Yoga as Medicine for Pregnancy
According to the American Cancer Society, approximately 233,000 new cases of prostate cancer will be diagnosed this year, and nearly 30,000 men will die from the disease. The diagnosis and treatment of prostate cancer in the United States has experienced significant shifts in the past few years, making management of cancer survivors challenging. One of the big changes in prostate cancer screening took place in 2011; the US Preventive Services Task Force recommended against routine prostate specific antigen, or PSA testing due to the level of potential harm such as psychological distress and complications from the biopsy. You can read a prior post about that here. New guidelines for providing care to prostate cancer survivors have been published by the American Cancer Society so that providers can better identify and manage the side effects and complications of the disease and recognize appropriate monitoring and screening of survivors.
In patients younger than 65 years of age, radical prostatectomy surgery is the most common intervention for prostate cancer. Long-term side effects of radical prostatectomy commonly include, according to the guidelines, urinary and sexual dysfunction. Urinary incontinence or retention can occur following prostatectomy, and sexual issues can range from erectile dysfunction to changes in orgasm and even penile length. Other common treatments, such as radiation and androgen deprivation therapy, are also related to urinary, sexual, and bowel dysfunction, as well as a long list of "other" effects.
These guidelines were developed using evidence as well as expert recommendations. Topics covered include obesity, physical activity, nutrition, smoking cessation, and surveillance. BMI as a baseline measure is recommended as a screening tool because elevated BMI is associated with poorer health outcomes. Increased physical activity can be related to higher quality of life and general benefits in cardiorespiratory health and physical function. Exercise recommendations are for 150 minutes/week of moderate intensity exercise or 75 minutes/week of vigorous intensity physical exercise. Nutrition suggestions include eating a diet that is rich in vegetables, fruits, and whole grains. Because smoking after prostate cancer increases the risk of recurrence, therapists should discuss the benefits of smoking cessation.
All of the above issues concern pelvic rehabilitation providers; patient concerns about sexual heath, urinary and bowel health, and subsequent pain in the abdomen or pelvis following treatment for prostate cancer are all conditions that can be positively influenced in the clinic. All of the lifestyle and wellness recommendations are ones that can be reinforced in pelvic rehabilitation, and patients can be referred for more specialized education when needed. To learn more about the care of men following prostate cancer, come to Male Pelvic Floor Function, Dysfunction, & Treatmentcontinuing education course in October in Tampa. Also, stay tuned for an announcement about our new Rehabilitation of the Post-Prostatectomy Course coming in 2015! (Send us an email if you are interested in hosting the new continuing education course that will focus on post-prostatectomy (and related issues) recovery!)
By accepting you will be accessing a service provided by a third-party external to https://www.hermanwallace.com/






































