Anorectal balloon catheter training is one of the most underrated but helpful treatments for people with pelvic floor symptoms related to bowel dysfunction. This is a tool that many clinicians don’t know about or are afraid to initiate with their clients. Clinicians wonder if clients will be receptive, how to use an anorectal balloon catheter efficiently, and frequently wonder what cases are appropriate for this specific modality. Anorectal balloon catheter training is a versatile treatment helping patients with pelvic floor conditions that stem from hyposensitivity or hypersensitivity in the rectal canal.
Rehab clinicians can use anorectal balloon catheters to help with defecation training, anorectal sensory training, coordination training, and resistance training that can improve symptoms for individuals with fecal incontinence, fecal urgency, and chronic constipation as well as other colorectal diagnoses. This modality can be used to improve the coordination between the pelvic floor muscles and the abdominal muscles to assist in defecation training. It also can help a patient learn what the urge to have a bowel movement should feel like, especially if they have altered sensation in the anal canal.
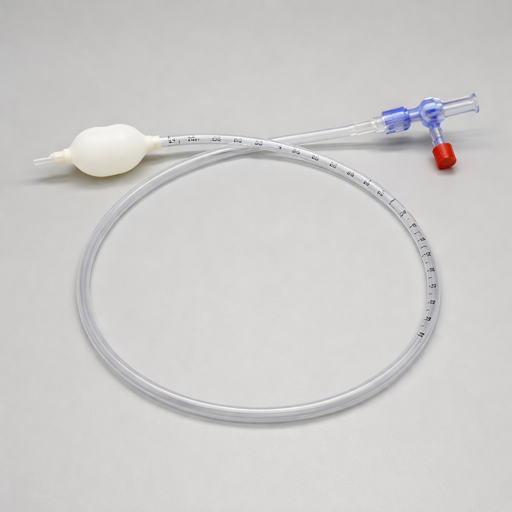
An anorectal balloon is a form of biofeedback to use with pelvic floor patients. During treatment, an anorectal balloon is placed in the rectal canal. The balloon can hold 400 mL but filling volumes are typically much lower. The balloon is then filled with air and the amount of air is altered in order to help retrain sensation in the anorectal area. Before implementing this treatment technique in a patient’s plan of care, there are a few steps a rehabilitation provider should take.
First, patients should be screened to make sure they are good candidates for this treatment. This includes internal muscle assessment of the rectal canal prior to implementing training. Detailed patient education on the purpose and procedure of training with an anorectal balloon catheter should be provided. Patients may have some experience with anorectal manometry and may need their therapist to differentiate how manometry testing is for assessment purposes, but balloon training is a biofeedback tool.
Once this treatment is decided upon, the therapist will begin by getting some baseline measurements. These include the first feeling of sensation of the balloon filling, the first urge to defecate, and then their maximum tolerance. These baselines give a provider information on how to proceed with treatment. It is helpful to have norms readily available to be able to compare your patient’s readings to. Caution should be taken when working with patients who have had lower bowel surgeries and pediatric patients, avoiding maximum values beyond a certain value.
With proper consideration of the baseline measurements of sensation levels, a treatment plan can be developed with the use of anorectal balloon training to improve sensation and awareness in the anorectal area. Sensation is trained via inflations and deflations of the balloon to assist in feedback to allow the patient to recognize what normal range values feel like.
Anorectal Balloon Catheters - Intro and Practical Application is a mini-course offered by Herman & Wallace to help providers feel comfortable screening patients for their eligibility for this intervention. The course will assist in helping practitioners to feel confident in providing this treatment with appropriate patients. This class is built with treatment in mind, and intended for therapists who have some exposure to the concept of anorectal assessment and treatment but want to learn more ways to apply this technique to their clients. This class includes didactic information and hands-on lab practice in the privacy of participant’s own space, to help bring this skill to their clinical practice. The next offering of this course is:
https://hermanwallace.com/continuing-education-courses/anorectal-balloon-catheters/

Have you ever gambled with what you thought was gas, only to find out that it was not? When my son was little, he asked me one day, “Mom did you ever try to fart, but it wasn’t really a fart?” At the time, I told him it was called a “shart.” Of course, being a little boy, he thought that was funny. However, being an adult and thinking you are passing gas, and it not be only gas can be mortifying. Think about how that could affect your quality of life and ability to go out in public. If you can’t trust your anal sphincters and anal canal to not know what you are letting go, it can be stressful!
What can lead to confusion and issues with sensation in this area? There are many different reasons that this area may not function ideally and be able to identify what is within the anal canal. These reasons can range from surgery in the area, radiation therapy, more minor procedures such as hemorrhoid treatment, and even chronically ignoring the urge to defecate. When sensation changes, the function of the sampling response and rectoanal inhibitory reflex (RAIR) or sampling response is changed.
The sampling response is when a small amount of fecal matter accumulates in the rectum, and a stretch occurs in the area. This then triggers a relaxation of the internal anal sphincter, and a contraction of the external anal sphincter that allows a small amount of the fecal matter to drop down into the anal canal. The contents of fecal matter are sampled, and it is determined if it is solid, liquid, or gas. If it is gas, then we can select to expel it; if it is liquid we usually respond with a stronger contraction of the external anal sphincter to hold it in. If it is solid, we can determine whether or not it is a good time to go. If it is, then we head to the restroom; if it is not, we engage the rectoanal inhibitory reflex and hold the stool until we decide there is a better time. You can see, if this sampling and identifying of the contents is off and not functioning properly, then we can have some issues arise and situations with “sharts” that would not be ideal!
We as pelvic rehab clinicians are the perfect people to help people when their sensation is not optimal, and they may have some issues with fecal and flatulence incontinence. Using rectal balloon catheters has been a game changer in my practice when working with these patients that have issues with sensation in their anal canal. The balloon retraining helps with retraining sensation in this area. I use it along with strengthening the pelvic floor and external anal sphincter; along with any manual therapy that may be needed, and defecation training. The addition of the balloons allows me to address sensation. The use of adding or removing small amounts of air in an inflated balloon allows the patient to learn what changes in sensation in the area feel like, which improves sensation and awareness of the contents within the anal canal. If you think about it, there isn’t another way to treat sensation inside of the anal canal. If we can retrain sensation, then we can make it less likely for a patient to think they are safe with expelling gas but be surprised when more comes out!
Join me for the May 17th course offering of Anorectal Balloon Catheters- Intro and Practical Applications. In this short course, you will learn how to use balloon catheters and even practice a lab using balloons. The purchase of a balloon is needed before the course so that you can participate in the labs. This course can change how you treat your patients who may suffer from fecal incontinence and constipation.
AUTHOR BIO
Allison Ariail, PT, DPT, CLT-LANA, BCB-PMD, PRPC
 Allison Ariail, PT, DPT, CLT-LANA, BCB-PMD, PRPC (she/her) has been a physical therapist since 1999. She graduated with a BS in physical therapy from the University of Florida and earned a Doctor of Physical Therapy from Boston University in 2007. Also in 2007, Dr. Ariail qualified as a Certified Lymphatic Therapist. She became board-certified by the Lymphology Association of North America in 2011 and board-certified in Biofeedback Pelvic Muscle Dysfunction by the Biofeedback Certification International Alliance in 2012. In 2014, Allison earned her board certification as a Pelvic Rehabilitation Practitioner. Allison specializes in the treatment of the pelvic ring and back using manual therapy and ultrasound imaging for instruction in a stabilization program. She also specializes in women’s and men’s health, including conditions of chronic pelvic pain, bowel and bladder disorders, and coccyx pain. Lastly, Allison has a passion for helping oncology patients, particularly gynecological, urological, and head and neck cancer patients.
Allison Ariail, PT, DPT, CLT-LANA, BCB-PMD, PRPC (she/her) has been a physical therapist since 1999. She graduated with a BS in physical therapy from the University of Florida and earned a Doctor of Physical Therapy from Boston University in 2007. Also in 2007, Dr. Ariail qualified as a Certified Lymphatic Therapist. She became board-certified by the Lymphology Association of North America in 2011 and board-certified in Biofeedback Pelvic Muscle Dysfunction by the Biofeedback Certification International Alliance in 2012. In 2014, Allison earned her board certification as a Pelvic Rehabilitation Practitioner. Allison specializes in the treatment of the pelvic ring and back using manual therapy and ultrasound imaging for instruction in a stabilization program. She also specializes in women’s and men’s health, including conditions of chronic pelvic pain, bowel and bladder disorders, and coccyx pain. Lastly, Allison has a passion for helping oncology patients, particularly gynecological, urological, and head and neck cancer patients.
In 2009, Allison collaborated with the Primal Pictures team for the release of the Pelvic Floor Disorders program. Allison's publications include “The Use of Transabdominal Ultrasound Imaging in Retraining the Pelvic-Floor Muscles of a Woman Postpartum.” Physical Therapy. Vol. 88, No. 10, October 2008, pp 1208-1217. (PMID: 18772276), “Beyond the Abstract” for Urotoday.com in October 2008, “Posters to Go” from APTA combined section meeting poster presentation in February 2009 and 2013. In 2016, Allison co-authored a chapter in “Healing in Urology: Clinical Guidebook to Herbal and Alternative Therapies.”
Allison works in the Denver metro area in her practice, Inspire Physical Therapy and Wellness, where she works in a more holistic setting than traditional therapy clinics. In addition to instructing Herman and Wallace on pelvic floor-related topics, Allison lectures nationally on lymphedema, cancer-related changes to the pelvic floor, and the sacroiliac joint. Allison serves as a consultant to medical companies and physicians.
Outside of work, Allison enjoys spending time with her family, caring for her animals, reading, traveling, and most importantly of all, being a mom! She lives in the Denver metro area with her family.










































